Brain health

Mental disorders, depression in particular, are becoming a global epidemic. Worldwide, more than 350 million people of all ages suffer from depression. Mental disorders result from a complex interaction between social, psychological and biological factors. One specific factor of interest is the relationship between the intestinal microbiota, the gut and the brain.
Influence microbiota beyond GI tract
The gut microbiota is essential for human health by protecting against pathogens and digesting food. However, the influence of the microbiota extends beyond the gastrointestinal (GI) tract, playing an important role in the bidirectional communication between the GI tract and the central nervous system (CNS), the so called microbiota- gut-brain axis.
Imbalances in the gut microbiota
For example, there is a clear association between imbalances in the gut microbiota and stress related disorders such as anxiety and depression. Also research has shown that certain animal behaviour appear to correlate with the composition of intestinal microbiota, and disruptions in microbial communities have been implicated in several neurological disorders.
Gut-brain-axis
The communication along this microbiota-gut-brain axis is bidirectional and complex involving neural, endocrine, immune, and metabolic pathways. In this respect it is important to highlight the role of the intestinal barrier. Impaired barrier function negatively influences hormones, immune cells and bacterial metabolites thus affecting microbiota-gut-brain communication.
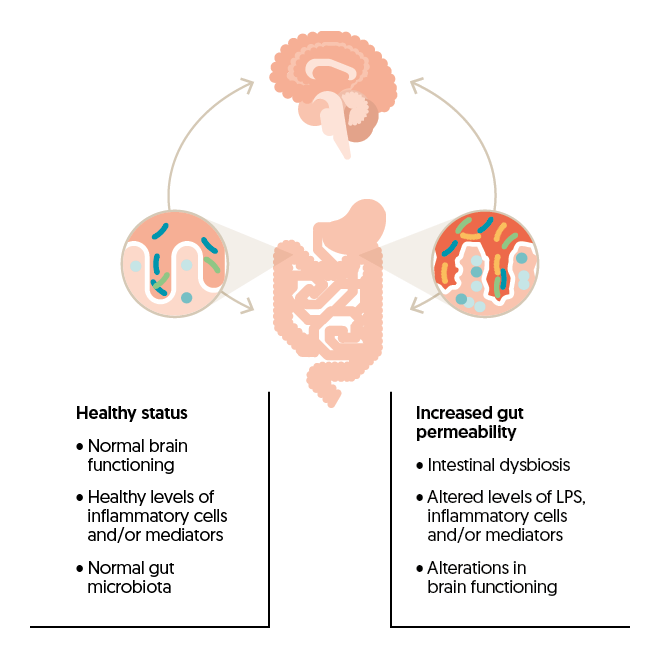
Probiotics and brain health
Research has shown that probiotics can positively influence the gut microbiota and intestinal barrier function. This raises the question whether probiotics can influence brain health as well. A question that seems to be answered with “yes”, as emerging evidence shows that probiotics are able to improve brain health (depression, anxiety, memory etc). Recent studies have demonstrated the ability of probiotics to influence the gut-brain axis and by this brain functioning.